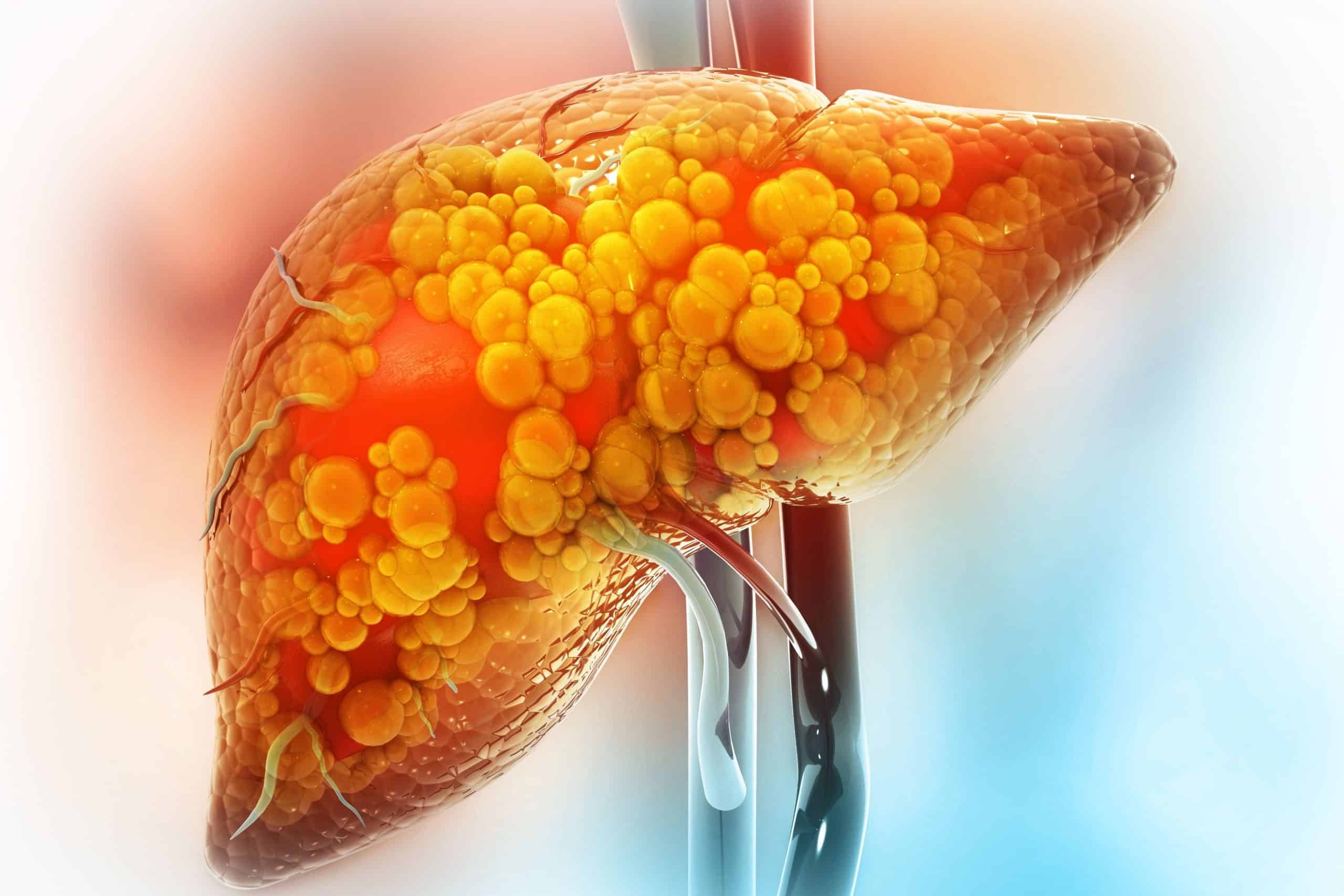
Overview
We all realise when we have a bit too much fat around the midriff, it is plain for all to see. What about having too much fat in your liver? You cannot see it or feel it, so most people do not even know it is present. Fatty liver disease is common in westernised cultures, with as many as one in ten people being affected. Fatty liver can be associated with the use of alcohol. This may occur with as little as ten ounces of alcohol ingested per week.
Fatty liver is characterised by a build up of fat in the liver, which replaces healthy tissue. It is normal for the liver to contain some fat naturally and this causes no symptoms. However, the fat build up can actually damage the liver and cause inflammation or even cirrhosis. Cirrhosis is scarring of the liver. Cirrhosis occurs in response to chronic damage to the liver. With mild cirrhosis, the liver can repair itself and continue to do its job. With more advanced cirrhosis, more and more scar tissue forms in the liver, making it impossible to function adequately. The liver carries out several essential functions, such as detoxifying harmful substances in the body, purifying the blood and manufacturing vital nutrients.
Types of Fatty Liver
There are two types of fatty liver disease that are not related to alcohol consumption.
| fatty liver disease (NAFLD) | Basic fatty liver is known as non alcoholic fatty liver disease, or steatosis, which refers to fatty infiltration. Simple fatty liver involves just the accumulation of fat in the liver cells with no inflammation or scarring. |
| Non alcoholic steatorrhoeic hepatitis (NASH) | Non alcoholic steatorrhoeic hepatitis involves the accumulation of fat in the liver cells as well as inflammation of the liver. The inflammatory cells can cause hepatocellular necrosis, which is death of the liver cells. Hepatitis is inflammation of the liver. This condition is far more harmful than simple fatty liver, as it can lead to scarring or fibrosis of the liver, which can result in irreversible scarring or cirrhosis. |
Causation
- Diet – consumption of excess calories and fat in an individual’s diet can cause fatty liver disease. The excess caloric intake overwhelms the liver’s ability to metabolise fat in a normal fashion, which results in fat accumulation in the liver. Severe malnutrition may also cause fatty liver, where the individual’s diet is protein deficient.
- Medical Conditions – non alcoholic fatty liver can be associated with type II diabetes, obesity, and high triglyceride levels in the blood, coeliac disease, and Wilson’s disease which is an abnormality of copper metabolism.
- There is evidence to suggest there may be a link between insulin resistance and the development of fatty liver. In this situation, although the body makes adequate insulin, there is an abnormality in the ability of cells to adequately use insulin to metabolise glucose. The relative excess of glucose is then stored as fat and can accumulate in the liver.
- Medications – such as:
- tamoxifen (Soltamox) – a prophylactic breast cancer medication;
- amiodarone injection (Nestorone) and oral amiodarone (Cordarone, Pacerone) – a treatment for heart rhythm problems; and
- methotrexate (Rheumatrex Dose Pack, Trexall) – treatment for severepsoriasis or sometimes rheumatoid arthritis as well as some cancers.
Symptoms
For the majority of patients, fatty liver is an asymptomatic condition. It is only when the liver manifests signs of inflammation, either non alcoholic steatorrhoeic hepatitis or alcoholic steatohepatitis, that the patient may experience symptoms. As with other types of hepatitis, the initial symptoms are non specific and include malaise, a generalized feeling of discomfort, illness, or lack of well being, fatigue, and upper abdominal fullness and discomfort. The patient may then progress to symptoms of liver disease such as jaundice, oedema, and ascites which is excess fluid in the peritoneal cavity in the abdomen. Jaundice is a yellow colour of the skin, mucus membranes, or eyes. The yellow colouring comes from bilirubin, a by product of old red blood cells.
Treatment
Treatment involves correcting the condition that causes fatty liver and providing supportive care. In fatty liver caused by alcoholism, the treatment is to cease drinking alcohol. If the cause is diet related, the treatment is to eat a healthy, well balanced diet. Vitamin and mineral supplements along with nutritional support may also be useful.
Cholesterol and triglyceride control are important both for treatment and to prevent progression of the disease from non alcoholic fatty liver to non alcoholic steatorrhoeic hepatitis, and from non alcoholic steatorrhoeic hepatitis to cirrhosis.
Cardiovascular exercise not only improves metabolism and promotes weight loss, the increase in muscle mass helps to sensitise the cells to insulin and reduces insulin resistance.